In this investigative report, our correspondent, SHAFA’ATU SULEIMAN, travelled across two states- Yobe and Sokoto to document the trajectories in the running of the country’s Primary Healthcare System. It independently looks at the failing approach and key successes of primary healthcare centres across the two states, and how weak health information systems make infrastructure planning reactive rather than proactive.
It was a sunny Thursday in March when Maryam Muhammad, a 32-year-old, made her way through Malluninnatati Primary Healthcare Center (PHC), one of the 400 facilities in Yobe State, Northeast Nigeria. She went straight to the nurse’s room section of the facility, where Aisha Saji, a Community Health Extension Worker (CHEW), was waiting to give her sick daughter medical attention.
The previous night, Maryam’s two-year-old daughter (name withheld) had been down with diarrhoea and feverish conditions. She had administered the common painkillers, but the baby’s condition has remained unstable and is deteriorating. This prompted her decision to rush the baby to the PHC.
The young mother is not a newcomer to the facility. She had always visited the PHC for medical treatment during her antenatal care, despite living a few kilometres from the State Specialist Hospital.
“This is Maryam’s favourite facility to receive medical treatment. We have the secondary facility behind us, but most parents prefer our facility because we have the capacity to attend to the outpatients,” said Saji, as she prepares to examine the little girl’s condition.
Maryam said, over time, she had built confidence in the way the health worker treated her, and the drugs she got were free.
“The health workers here pay attention to every detail of their patients. My house is closer to the specialist hospital, but I prefer to come down here,” she adds.
Across Yobe State, this investigation revealed that residents have built trust in the health system at the grassroots level. They frequently access the PHCs rather than going to the secondary facility. Data showed that Yobe paraded no fewer than 486 PHC facilities that are publicly owned. At the secondary health care level, 40% (12 ) of 30 health facilities are publicly owned, while 18 (60%) are privately owned. The only tertiary health facility in the State is publicly owned.
Primary healthcare workers say they’re seeing a change in the statistics, with the numbers of women attending antenatal care appointments and giving birth in the facility having risen steeply.
Muhammad Goni, a Health Monitoring and Evaluation Officer at Forestry PHC in Damaturu, the state capital, says the facility not only received the patient’s complaint but also conducted a preliminary test before beginning the treatment.
“We have helped discover a lot of tuberculosis cases because of the way we approach treatment for most outpatients. We refer such cases to either the Specialist hospital or the State Teaching hospital for proper treatment and evaluation,” he explained.
THE GRIEVING STORIES FROM SOKOTO PHCs
While Yobe residents experienced a ‘one-stop’ at primary healthcare facilities in accessing a more satisfying service to their health challenges, most Sokoto residents say they traverse across several health facilities before their ailments could be managed or treated.
Ismaila Hussaini, 53, recounts the harrowing experience of how he lost his eighteen-year-old boy while trying to get medical help after he sustained a headbutt injury during a football game with his peers.
Hussaini had rushed his critically injured son to Bunkari Primary Healthcare Centre (PHC) in his Binji Local Government Area of Sokoto State, Northwest Nigeria, but there were no medical personnel to attend to him.
“When we arrived at the facility at about 6 pm, the security man told us that the Community Health Environmental Worker (CHEW) had closed from duty for the day.”
He said his son was later moved to another PHC, but the facility lacked the capacity to handle the situation.
“We couldn’t get the medical attention that we needed after the stopover at two different facilities. The only option was to travel to Sokoto, a distance of about 30 Kilometres away from the community, where he could be treated at either the State Specialist Hospital or perhaps, the Usmanu Danfodiyo University Teaching Hospital.
“The journey worsened his condition because he bled on the head throughout our journey. He eventually gave up the ghost before we could get to Sokoto.” Hussein recounts.
A similar fate also befell Hajatu Sabaru, a 26-year-old housewife who had developed severe abdominal pain and difficulty breathing in her seventh month of pregnancy.
Her husband, Jamilu, was a peasant farmer with no money to hire a private vehicle. Jamilu was helpless as his wife’s condition worsened. The nearest health facility was in Kwannawa, about 15 kilometres from the Kwannawa community, where the couple lived.
Jamilu immediately contacted a community leader, who arranged a vehicle to convey Hajatu to the health facility.
The couple travelled several kilometres before finally reaching the clinic, while the community leader covered the cost of transportation and medical treatment.
Although she survived, she lost her stillborn baby. While still reflecting on the ordeal, Hajatu said she feared she would not survive. “I thought I was going to die, but thank God I survived that terrible experience,” she said.
Both Hussein and Hajatu are paradoxes of thousands of patients shuttled daily from under-equipped PHCs just to be alive.
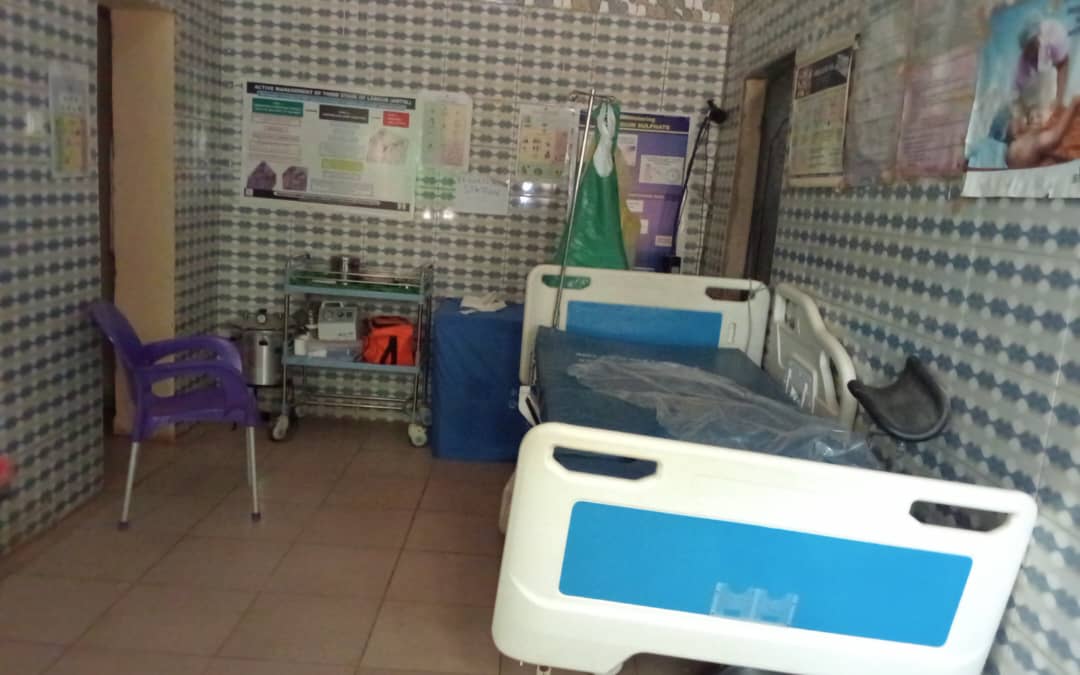
In March, this investigation visited a cross-section of Primary Healthcare centres across Yabo, Dange Shuni, and Binji Local Government Areas. The outcome of the visit was an eyesore. From broken ambulances to damaged beds and absent laboratories, the story repeats itself across its 244 wards, where the majority of the health facilities are located.
In 2024, the reported rate of maternal mortality in Sokoto state stands at 1,200 deaths per 100,000 live births, one of the highest rates in Nigeria, where the national average is 512 deaths per 100,000.
A 2024 assessment by Orodata CheckmyPHC indicated that in Sokoto State, over 60 percent of its 793 registered PHCs lack basic infrastructure, staffing, and supplies necessary to deliver even minimal care.
Mohammed Dahiru, a statistician and data analyst, admits that the state’s maternal health indicator and other services like immunisation and family planning services have created a wider gap in the state’s health system.
Dahiru agrees that Sokoto is one of the few states contributing to Nigeria’s highest number of children with zero doses in the world, with only 71% of children receiving the first dose of the diphtheria, tetanus, and pertussis (DTP1) vaccine, compared to the global average of 89%.
 “This is a state where over 80 percent of the population lives in rural areas. The collapse of PHC services is dangerous for the well-being of the citizens,” he further laments.
“This is a state where over 80 percent of the population lives in rural areas. The collapse of PHC services is dangerous for the well-being of the citizens,” he further laments.
This investigation further revealed that only 12 percent of PHCs in Sokoto state have functioning ambulances; most referrals are made without transport support, forcing families to embark on deadly journeys to distant city hospitals in emergency cases.
THE SOKOTO’S OVERBEARING SYNDROME
Sokoto, the State capital, is home to two of the most significant federal medical institutions. These include: Usmanu Danfodiyo University Teaching Hospital, and Federal Neuropsychiatric Hospital, which is approximately located at Kware, a few kilometres from the state capital.
However, public analysts say residents’ overbearingness on these facilities is “quite alarming and disturbing.”
Anas Sabir, Chief Medical Director of Usmanu Danfodiyo University Teaching Hospital, Sokoto, said most residents bypass the referral orders due to a lack of confidence in the primary healthcare services in the state.
“In the health system, we have a structure of primary, secondary, and tertiary. The ideal is for a patient to explore health services right from the PHC before he or she can be referred to either secondary or tertiary facilities.
“But that referral chain is frequently bypassed in Sokoto, forcing the hospitals to handle basic cases like malaria, headache, among others,” Sabir explains.
He outlined several interlinked factors behind the decay of PHC infrastructure in Sokoto State and across Nigeria.
According to him, only 5 to 6% of the national health budget is allocated to PHC services,” he said, “far below the Abuja Declaration target of 15%. At the state level, health spending is still skewed toward tertiary care.”
WHY YOBE LEADS BUT SOKOTO LAGS?
A recent comparative Health systems analysis obtained by this investigation shows how health financing, service delivery quality, data systems and accountability, immunisation coverage, and community engagement are factors that boost efficiency in the health sector.
The Performance Benchmark measured by the PHC Leadership Challenge award, in which Yobe State ranked 1st nationally, while Sokoto State fell among the lowest-performing states, was promoted by the Nigeria Governors’ Forum in partnership with the National Primary Health Care Development Agency, among other partners.
When measuring both Yobe and Sokoto financing and budget prioritisation, it said Yobe’s success was tied to consistent investment in PHC systems and reforms, an approach which aligned with national frameworks like the Health Sector Renewal Initiative.
The NGF noted that winning states like Yobe had demonstrated “sustainable financing” and accountability systems. “Yobe leveraged performance-based incentives, reinvesting its $1.2 million award into PHC strengthening.
On its part, Sokoto’s structural funding was said to have suffered from underfunding and poor budget execution, with many states, including Sokoto, falling below the 15% Abuja Declaration benchmark.

The reports say Yobe ties funding to measurable outcomes, while Sokoto shows funding with weak implementation linkage, especially in infrastructure development.
The report further praised Yobe’s rapid gains through System Reform, saying Routine Immunisation coverage in Yobe improved dramatically, “From 9% to 65% after adopting integrated PHC reforms and funding models. “This reflects strong outreach systems, community-level engagement, and effective partner coordination,” the report further said.
It adjudges Sokoto as remaining one of Nigeria’s zero-dose and under-immunised states due to its structural barriers, ranging from low female health decision autonomy, weak last-mile service delivery, as well as cultural and access barriers.
The NGF specifically cited the use of data for decision-making, strong accountability frameworks, institutional structure with a functional PHC management board as part of the Yobe driving success, while Sokoto’s PHC system was said to have faced leadership disruptions, weak coordination between agencies, and limited evidence of real-time data use in planning and budgeting.
On the community engagement, it was indicated that Sokoto has a weak budget execution and funding inefficiency, less immunisation coverage, and demand barriers, while its healthcare institution structure also suffered instability and weak data systems.
“WHAT WE DO DIFFERENTLY”
Dr. Babagana Kundi Machina, Executive Secretary, Yobe State Primary Healthcare Development Board, said Yobe’s primary health breakthrough is largely due to an “all-of-government approach, recalling that every level of government and stakeholder was actively involved- from the top leadership to the field workers.
He said that the state also introduced monthly task force meetings on immunization, chaired by the governor, where performance data across local governments is reviewed and decisions taken. “We present expenditure, performance, and gaps transparently. This level of accountability ensures that both the government and local authorities take responsibility,” he explained.
He added that the State’s PHC funding is now ring-fenced, reducing the risk of mismanagement and ensuring funds are used strictly for healthcare delivery.
Dr. Musa Usman Matazu, a Health Systems Consultant working with the Gates Foundation, also corroborates Machina’s submission by reflecting on the strategic partnerships between the Yobe State Government and the Gates Foundation.
He noted how the partnership has significantly transformed the state’s healthcare system, “and reversing years of poor performance and weak infrastructure.”
“Before the MOU, the system suffered from poor infrastructure, weak accountability, unreliable data, and low service utilization. But this investment has been catalytic in reversing those negative trends,” he said.
He attributed part of the success to technically competent leadership, particularly having health professionals rather than politicians heading the sector.
The consultant disclosed that the state has achieved over 98 percent cold chain coverage, ensuring vaccines reach even the most remote communities.
“This has improved public trust and increased immunization uptake. Every facility offering routine immunization now has access to potent vaccines. That was not the case before,” he added.
BEYOND OR ABOVE THE STANDARD?
According to the National Primary Health Care Development Agency, a body that oversees the management of the primary healthcare system in Nigeria, a standard (PHC) must be equipped with essential medical tools such as weighing scales, thermometers, stethoscopes, blood pressure monitors, and examination lights.
In addition to adequate equipment, each PHC should be staffed with at least one doctor, two nurses or midwives, and some Community Health Extension Workers (CHEWs) to ensure comprehensive service delivery.
It also mandates the primary healthcare centres to provide a broad range of services, including immunizations, antenatal and postnatal care, family planning, treatment of common ailments, and health education.
To serve communities effectively, these facilities must be located within a reasonable distance from the population they serve, in line with the World Health Organization’s recommendation of one PHC per 10,000 people.

Dr Kingsley Onoja, a medical practitioner, agrees with the outlines but said most PHCs in Sokoto and elsewhere in the State are operating below the agency’s specifications.
“The PHCs are expected to operate daily, with provisions for emergency services to ensure uninterrupted access to essential healthcare because they serve as the first point of contact for any patient, Onoja notes.
“But in the Sokoto case, many residents have lost confidence in the PHCs because they lack these basic amenities and essential medicines, which are the factors that severely hamper service delivery, ” said Abubakar Tasiu, a retired health worker.
“When PHCs are weak or non-functional, patients bypass them and flood secondary and tertiary hospitals for conditions that could easily be managed at the community level,” Tasiu noted.
The Sokoto State Commissioner in charge of the Health ministry, Dr. Faruk Abubakar Wurno, said the decay in the primary healthcare system was a result of mispriorities by the previous administrations.
He said the current government has launched a state-wide needs assessment, which exposed glaring gaps and helped develop a strategic framework to tackle challenges at the primary, secondary, and tertiary healthcare levels.
“This government is not just reacting; we are planning. And that’s the game-changer, because health is wealth,” he concluded.
“WHAT NEEDS TO BE DONE”
Dr Matazu says the lack of accountability and mismanagement in the running of the primary healthcare system is affecting the performance of PHCs across the country.
He also emphasized the role of traditional institutions and community leaders in improving healthcare access. “The regular engagement with emirs, district heads, and community volunteers will help address resistance and improve awareness.
“You can build modern facilities, but if communities don’t trust or use them, they become useless. That is why community engagement is critical,” Dr. Matazu said.
He described Yobe as a model for effective coordination among development partners, noting that stakeholders work collectively rather than competitively.
“You don’t play politics with health. When professionals lead, they understand priorities like human capital development, not just visible infrastructure,” he said.
He criticized the common practice of prioritizing buildings over skilled personnel, describing it as a major setback in Nigeria’s health system.
Drawing from his experience, the consultant stressed that Nigeria has sufficient resources to fix its health system but is hindered by corruption and poor prioritization.
“We have money, but it is mismanaged. Investing in human capital is what sustains any system, not just constructing buildings,” he stated.
Dr Onoja, on his part, highlighted issues of fragmented governance. “PHCs are managed by local governments, many of which lack the capacity, funding, and autonomy to maintain them.”
“Several audits by the ICPC and civil society organizations have uncovered ghost projects and misappropriated funds intended for PHC revitalization.” Onoja
But for many health analysts, Sokoto’s challenges mirror a broader crisis, where more than 60% of Nigeria’s rural population lacks a functional primary healthcare facility, with less than half fully equipped.
* This article was first published on www.thecable.ng


